AI Will Not Replace Doctors, But It May Drastically
Change Their Jobs
This op-ed posits that in the same
way that the finance industry adopting technology and its subsequent
infiltration of their dynamics changed the roles of everyone employed, the same
thing is bound to happen to healthcare, which has historically been one of the
slowest industries in adopting and integrating technology into practice. This
is because of a human-centric service model, an intense educational background
needed to practice, a deep-rooted culture, and a large and complex industry.
Important pull-quote: “There’s not going to be an AI that solves
health care — just like there isn’t one solution to all retail (groceries,
clothing and music all took very different paths to digitization) or all
marketing (as the MarTech 5000 technology landscape shows). Rather, based on
one process within one specialty at a time, automated systems are showing up
and ready for prime time: identifying abnormal chest x-rays, diagnosing common
pediatric diseases, analyzing lymph node slides in pathology, detecting eye
disease early on and assessing mental health.”
Replacing doctors [ Medical Economics Journal, February
10, 2019 edition , Volume 96, Issue 3 ]
https://www.medicaleconomics.com/view/replacing-doctors
Nurse Practitioners (NPs) have
independent practice rights in 22 states and DC. While physician assistants
(PAs) still require a formal agreement with a supervising physician, the
American Academy of Physician Assistants is advocating that a collaborative
agreement with a physician no longer be necessary to practice.
According to the American
Osteopathic Association (AOA), physicians average more than 12,000 patient-care
training hours, while NPs average more than 500 and PAs over 2,000.
Will doctors be replaced by algorithms?
https://scopeblog.stanford.edu/2018/09/11/will-doctors-be-replaced-by-algorithms/
Important pull-quote: “Without a doubt, algorithms will play a
vital and growing role in health care. However, while they may soon become
superhuman at performing certain tasks, algorithms do not have the general
intelligence that people do, nor the ability to empathize with patients. It’s
this unique combination that enables us, as care professionals, to work
together effectively and to draw from clinical and emotional experience to
build genuine, healing relationships with our patients. When we’re at our best,
this can be powerful medicine.”
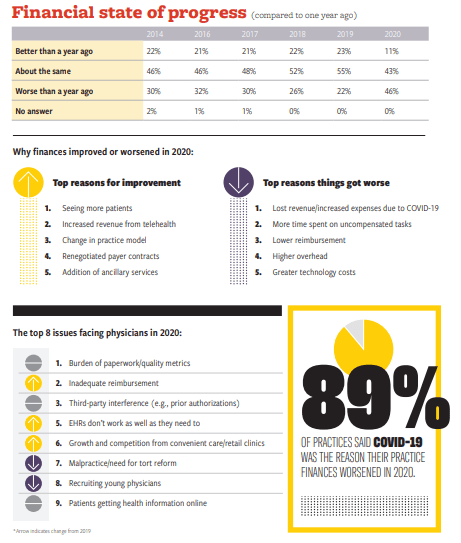
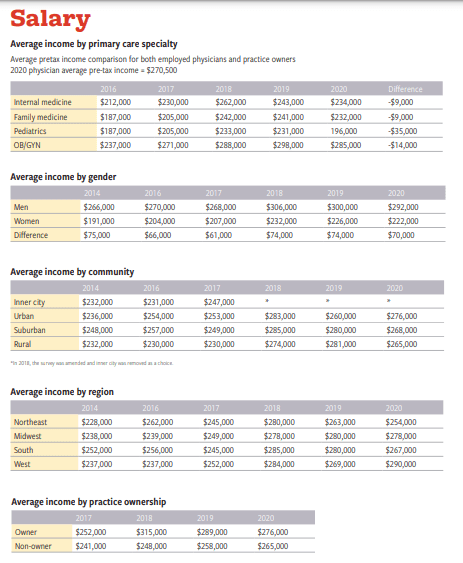
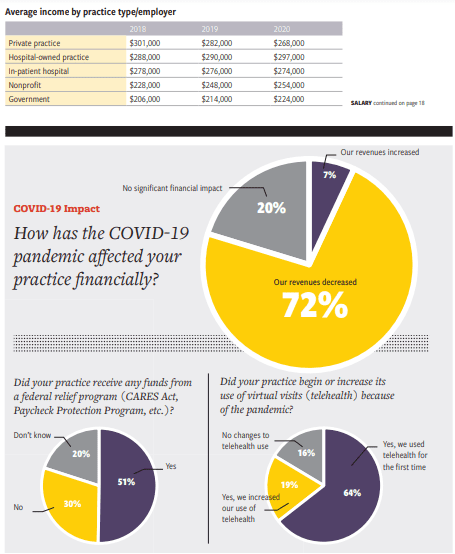
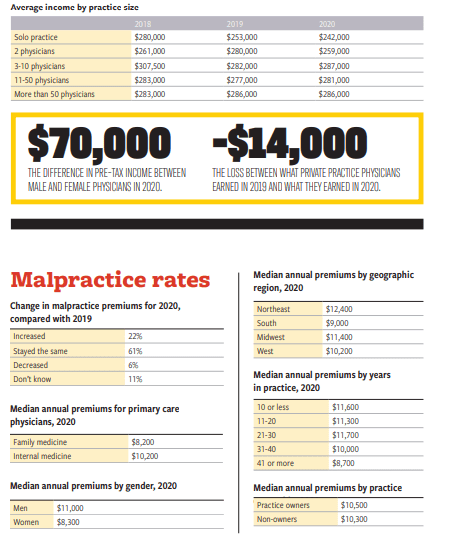
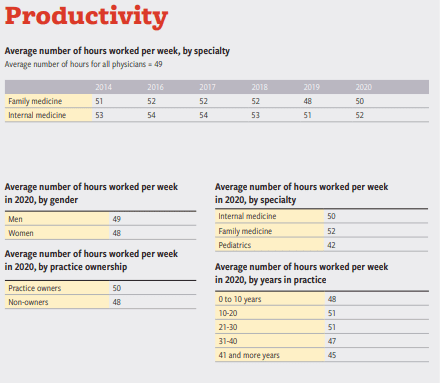
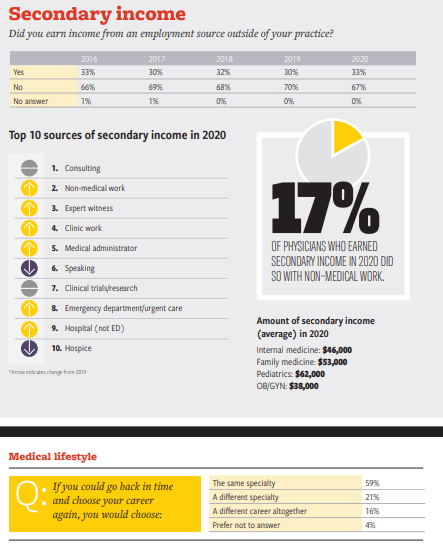
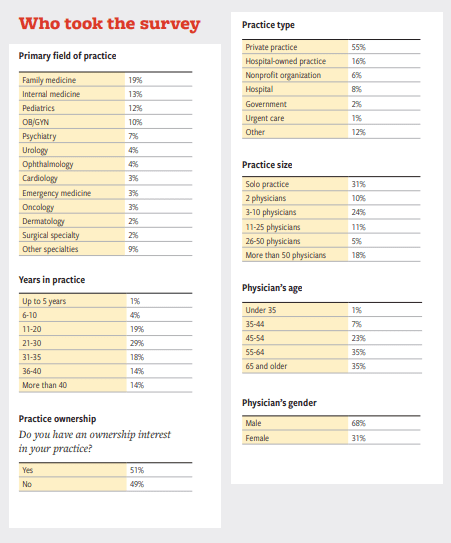
Medical Economics’ Survey Results on Salary, Malpractice,
and Productivity
https://cdn.sanity.io/files/0vv8moc6/medec/f54a0e50ca7637db190edbf026dea2560260badf.pdf